
Cardiac tamponade is a life-threatening medical emergency that requires immediate recognition, rapid diagnosis, and timely medical intervention to prevent fatal complications. This condition occurs when fluid accumulates in the pericardial sac surrounding the heart, compressing it and impairing its ability to pump blood efficiently. Consequently, cardiac tamponade reduces cardiac output and disrupts normal circulation, which can quickly lead to shock and organ failure.
In this comprehensive blog, we elaborate on cardiac tamponade in detail, covering its causes, symptoms, epidemiology, diagnostic methods, and treatment options. Additionally, we emphasize the importance of early detection and clinical awareness.
What is cardiac tamponade
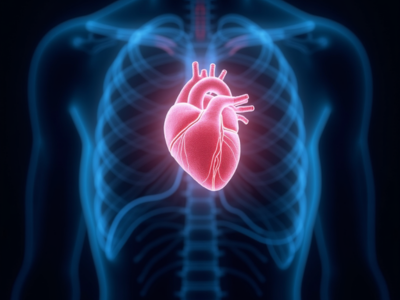
Cardiac tamponade develops when excess fluid collects in the pericardial space, the thin sac that encloses the heart. Under normal conditions, this space contains a small amount of fluid that reduces friction during heartbeats. However, when fluid accumulates rapidly or in large quantities, it exerts pressure on the heart.
As a result, the heart chambers cannot expand properly during diastole, which significantly limits blood filling. Consequently, cardiac tamponade decreases stroke volume and cardiac output. Furthermore, reduced blood flow affects oxygen delivery to vital organs, including the brain and kidneys. In acute cases, cardiac tamponade develops suddenly and progresses rapidly, often becoming fatal without immediate treatment. In contrast, chronic cardiac tamponade develops slowly, allowing the body to temporarily compensate, although it remains equally dangerous if untreated.
Epidemiology and Market Insights
Understanding the epidemiology of cardiac tamponade provides valuable insights into its clinical burden and market growth. The incidence of cardiac tamponade is approximately two cases per 10,000 population in the United States. Although relatively rare, cardiac tamponade remains a critical condition due to its high mortality risk if untreated. Additionally, around 2% of penetrating injuries are reported to result in cardiac tamponade. Therefore, trauma centers frequently encounter cardiac tamponade in emergency settings, particularly in cases involving chest injuries.
In pediatric populations, cardiac tamponade is more common in boys than in girls, with a male-to-female ratio of approximately 3:0. In contrast, among adults, cardiac tamponade appears slightly more prevalent in men than in women. Clinical observations indicate a male-to-female ratio of 1.26:1 in certain referral centers, while other level 1 trauma centers report a ratio closer to 1.3:1. These variations highlight demographic differences in cardiac tamponade occurrence. Moreover, a major factor driving the growth of the cardiac tamponade market is the increasing prevalence of cardiovascular diseases. In the United States, a heart attack occurs approximately every 40 seconds, underscoring the widespread burden of heart disease.
Each year, nearly 805,000 individuals experience a heart attack. Of these cases, around 605,000 are first-time heart attacks, while approximately 200,000 occur in individuals with a prior history. Furthermore, about one in five heart attacks is silent, meaning the damage occurs without noticeable symptoms. As a result, undiagnosed cardiac conditions may increase the risk of complications such as cardiac tamponade.
Causes of Cardiac Tamponade
Cardiac tamponade arises from various underlying conditions that lead to fluid accumulation in the pericardial sac. Although the mechanisms differ, all causes ultimately increase intrapericardial pressure.
- Trauma and Injury: Trauma is one of the most common causes of acute cardiac tamponade. For instance, penetrating injuries such as stab wounds or gunshot wounds can directly introduce blood into the pericardial space. Similarly, blunt chest trauma from accidents can damage cardiac structures and cause internal bleeding.
- Medical Conditions: Several systemic diseases contribute to cardiac tamponade by causing inflammation or fluid accumulation. For example, cancers such as lung or breast cancer can metastasize to the pericardium, leading to malignant effusion.
- Heart-Related Conditions: Cardiac tamponade may also develop due to primary heart conditions. For instance, a heart attack can weaken the heart muscle and lead to rupture, allowing blood to leak into the pericardial space.
- Medical and Surgical Procedures: Certain medical procedures can inadvertently cause cardiac tamponade. For example, catheter-based interventions, pacemaker insertions, or cardiac surgeries may lead to accidental perforation of the heart or surrounding vessels.
Symptoms of Cardiac Tamponade
Recognizing cardiac tamponade symptoms early can save lives. However, symptoms may vary depending on how quickly fluid accumulates.
Common Symptoms
Initially, patients may experience:
- Chest pain radiating to the neck, back, or shoulders
- Shortness of breath
- Rapid breathing
- Fatigue and weakness
These symptoms often worsen with physical activity or lying flat.
Advanced Symptoms
As cardiac tamponade progresses, more severe signs appear. These include:
- Low blood pressure
- Rapid heart rate
- Dizziness or fainting
- Confusion or restlessness
Moreover, a classic clinical presentation known as Beck’s triad includes low blood pressure, distended neck veins, and muffled heart sounds. Therefore, any combination of these symptoms requires urgent medical attention.
Diagnosis of Cardiac Tamponade
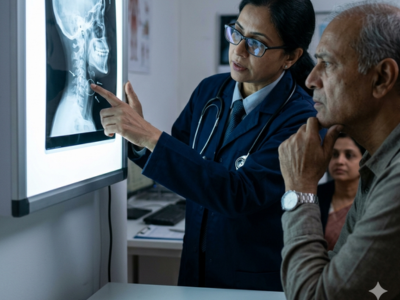
Diagnosing cardiac tamponade involves a combination of clinical evaluation and imaging techniques. Early diagnosis is critical, as delayed recognition can lead to severe complications.
- Clinical Examination: Doctors begin by assessing vital signs and observing physical symptoms. For instance, low blood pressure, rapid heart rate, and elevated jugular venous pressure raise suspicion of cardiac tamponade. Furthermore, auscultation may reveal muffled heart sounds, while peripheral signs such as cold extremities indicate poor circulation.
- Imaging Techniques: An echocardiogram is the most important diagnostic tool for cardiac tamponade. It allows doctors to visualize fluid accumulation and assess its impact on heart function in real time. Additionally, an electrocardiogram may show electrical alternans, a pattern caused by the swinging motion of the heart in fluid. Chest X-rays and CT scans provide further confirmation by revealing an enlarged cardiac silhouette or fluid collection.
- Laboratory Tests: Although not definitive, blood tests can help identify underlying causes such as infection, inflammation, or metabolic disorders. Therefore, a comprehensive diagnostic approach ensures accurate identification of cardiac tamponade.
Treatment of Cardiac Tamponade
The treatment of cardiac tamponade focuses on relieving pressure on the heart and addressing the underlying cause. Since cardiac tamponade is a medical emergency, immediate action is necessary.
- Emergency Stabilization: Initially, patients receive oxygen therapy and intravenous fluids to maintain blood pressure. In some cases, medications are administered to support heart function and stabilize circulation.
- Pericardiocentesis: Pericardiocentesis is the primary treatment for cardiac tamponade. During this procedure, a needle is inserted into the pericardial space to remove excess fluid. As a result, pressure on the heart decreases rapidly, restoring normal function. This procedure is often guided by ultrasound to ensure accuracy and safety. In many cases, it provides immediate relief and stabilizes the patient.
- Surgical Management: In severe or recurrent cases, surgical intervention becomes necessary. Procedures such as pericardial window creation allow continuous drainage of fluid, preventing reaccumulation. Additionally, thoracotomy may be performed in traumatic cases to repair cardiac injuries and remove clots. Partial removal of the pericardium may also be considered in chronic conditions.
- Treating the Underlying Cause: Long-term management involves addressing the root cause of cardiac tamponade. For instance, infections require antibiotics, while cancer-related cases may need chemotherapy or radiation therapy. Similarly, anti-inflammatory medications help manage pericarditis, reducing the risk of recurrence. Therefore, a targeted treatment approach improves overall outcomes.
Future Insights
Cardiac tamponade is a critical medical condition that demands urgent attention and effective management. It occurs when fluid accumulation compresses the heart, impairing its ability to pump blood efficiently. As discussed, cardiac tamponade can result from trauma, medical conditions, or procedural complications. Its symptoms range from mild discomfort to life-threatening shock, depending on severity.
Importantly, epidemiological data highlight its clinical significance, while rising cardiovascular disease rates continue to increase associated risks. Early diagnosis using echocardiography and prompt treatment through pericardiocentesis or surgery can save lives. Therefore, understanding cardiac tamponade and recognizing its warning signs plays a vital role in improving patient outcomes and reducing mortality.